Analysis by Keith Rankin.
Last week I published charts for six countries showing excess deaths triggered by all seasonal and respiratory maladies, not just Covid19. The other main conditions that show up in excess deaths are epidemic influenza and the group of endemic viral infections commonly known as the ‘common cold’. Here I look at four more countries.
I finished by speculating that countries which show the highest rates of seasonal mortality are more likely to be those countries with the highest statistical life expectancies.
Israel
Israel is such a country, with a life expectancy of 83, and which experiences winter mortality rates typically at 40 percent above summer rates.
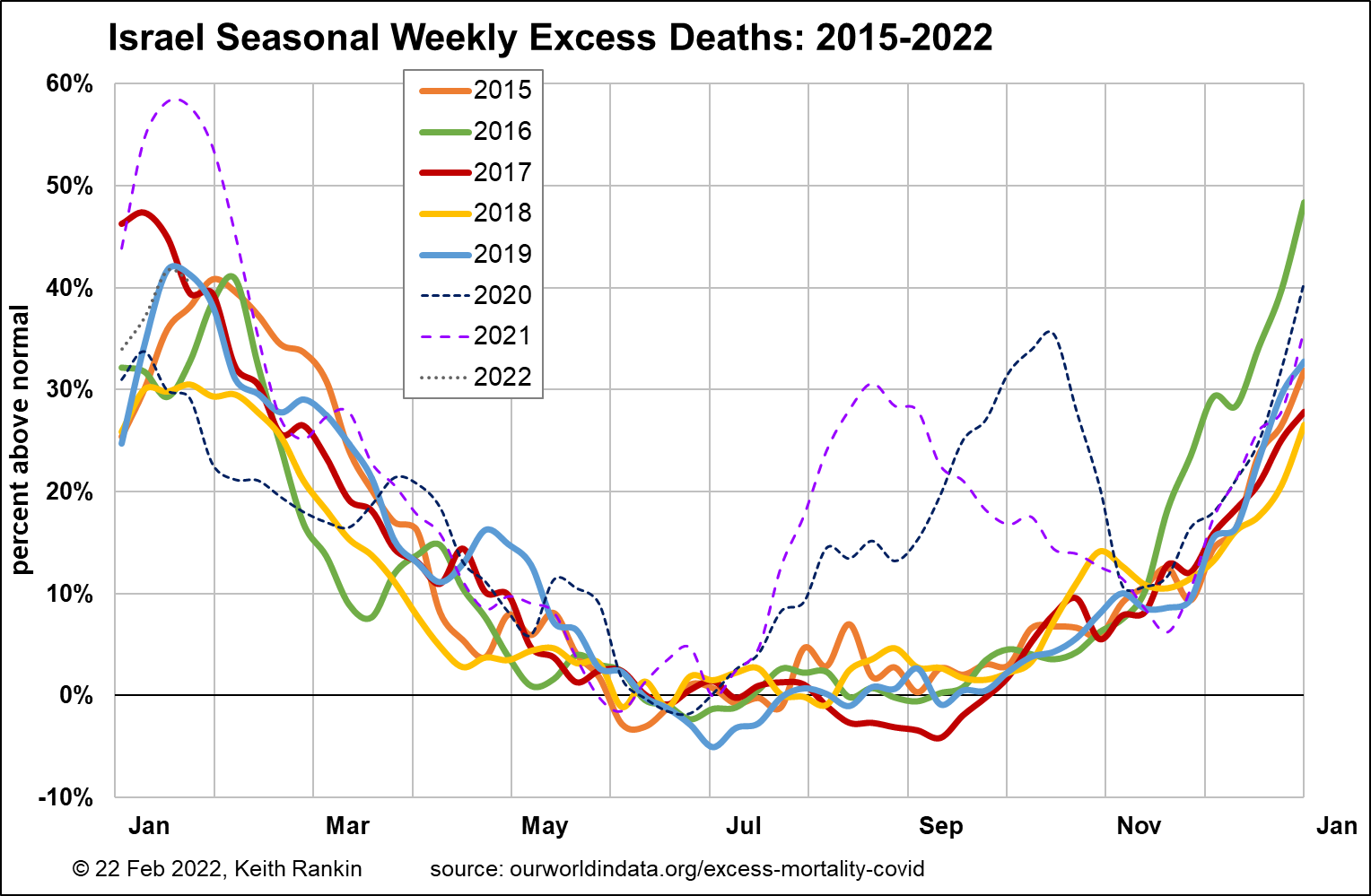
Israel’s mortality generally peaks in January, where in every pre-covid January except 2018 and 2020, mortality rates were 40% or more above the summer mortality norm.
It looks like endemic respiratory conditions trigger winter mortality rates around 30% above summer norms. In Israel, this may be exacerbated by Jewish cultural norms which see many socialisation events in winter. Most particularly, these deaths happen in winter because comparatively few deaths happen directly from heart conditions, strokes, and cancers.
The biggest Covid19 mortality wave in Israel – in January 2021 – is much like a bad flu wave. The other two waves of covid deaths peaked on October 2020 (original variant) and August 2021 (delta variant).
Re Omicron in Israel, see my Covid Omicron in Two High Immunity Countries, and this chart in particular. Omicron hit Israel well after its Delta wave was over. Excess deaths were falling at a time that covid cases, and people dying with covid, were rising dramatically. The context of ‘excess deaths’ in January 2022, however, is that of normally high January epidemic and seasonal endemic deaths. In the chart above, we see the Omicron covid wave matching the influenza wave of January 2019.
Israel is the best known country to offer fourth vaccination shots. It’s hard to judge their success, because Omicron deaths were high; as high as flu deaths would have been in another year. But there was no flu season in Israel this winter.
Norway
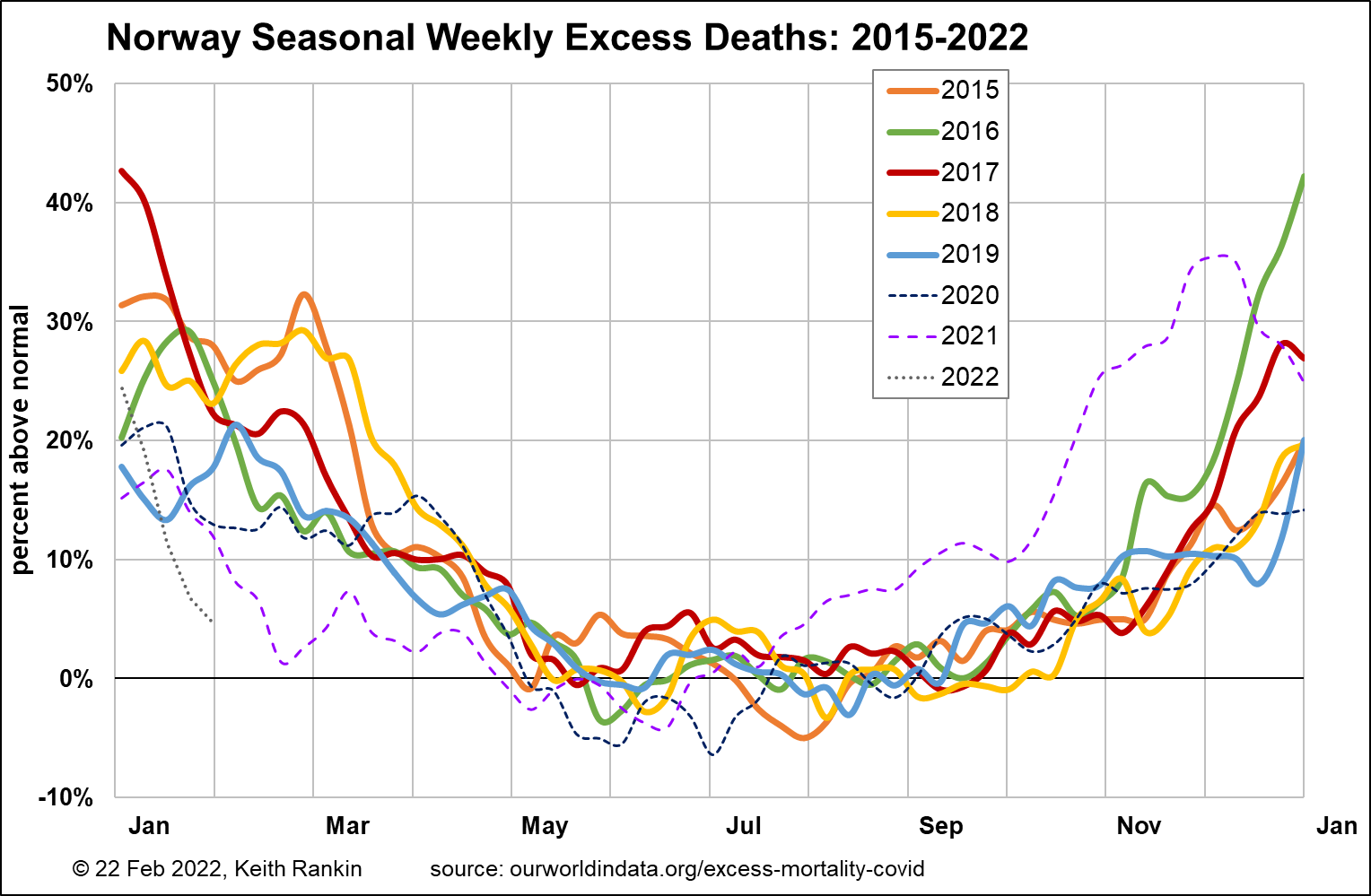
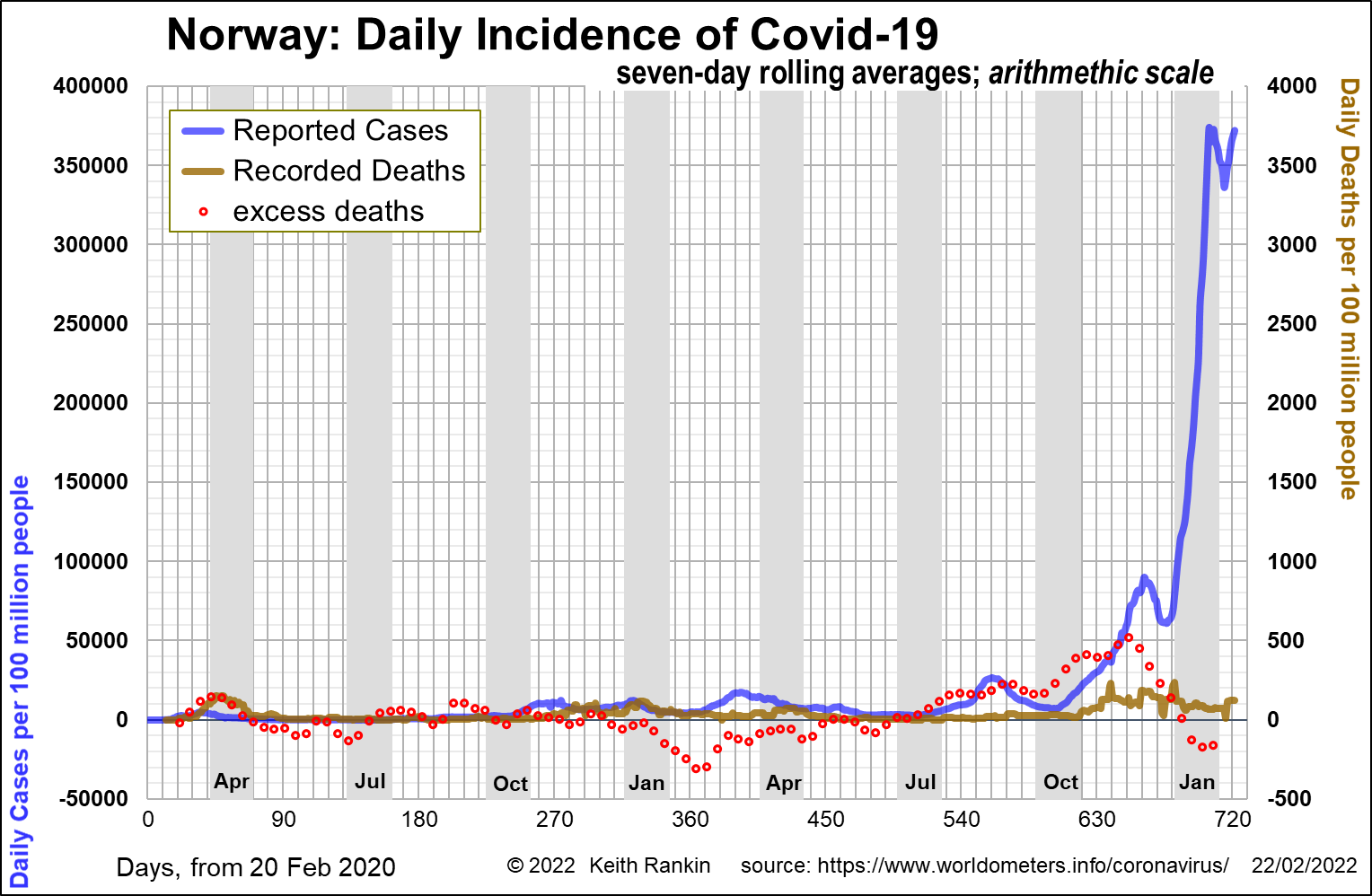
Norway is unusual in that it shows no classic covid mortality wave. This is largely due to effective public health measures. Nevertheless, Norway saw substantial excess mortality during the Delta period, in large part older people dying then who, in more normal circumstances, would have died in the winter of 2019/20 or the winter of 2020/21.
Norway was highly affected by Omicron, and, earlier than most other countries, getting high numbers of Omicron cases at a time when when there were already large numbers of Delta cases.
Excess deaths in Norway have fallen markedly during the Omicron period in Norway, despite massive numbers of cases. Indeed, excess deaths in January 2022 are well below those of previous Januarys.
United Kingdom
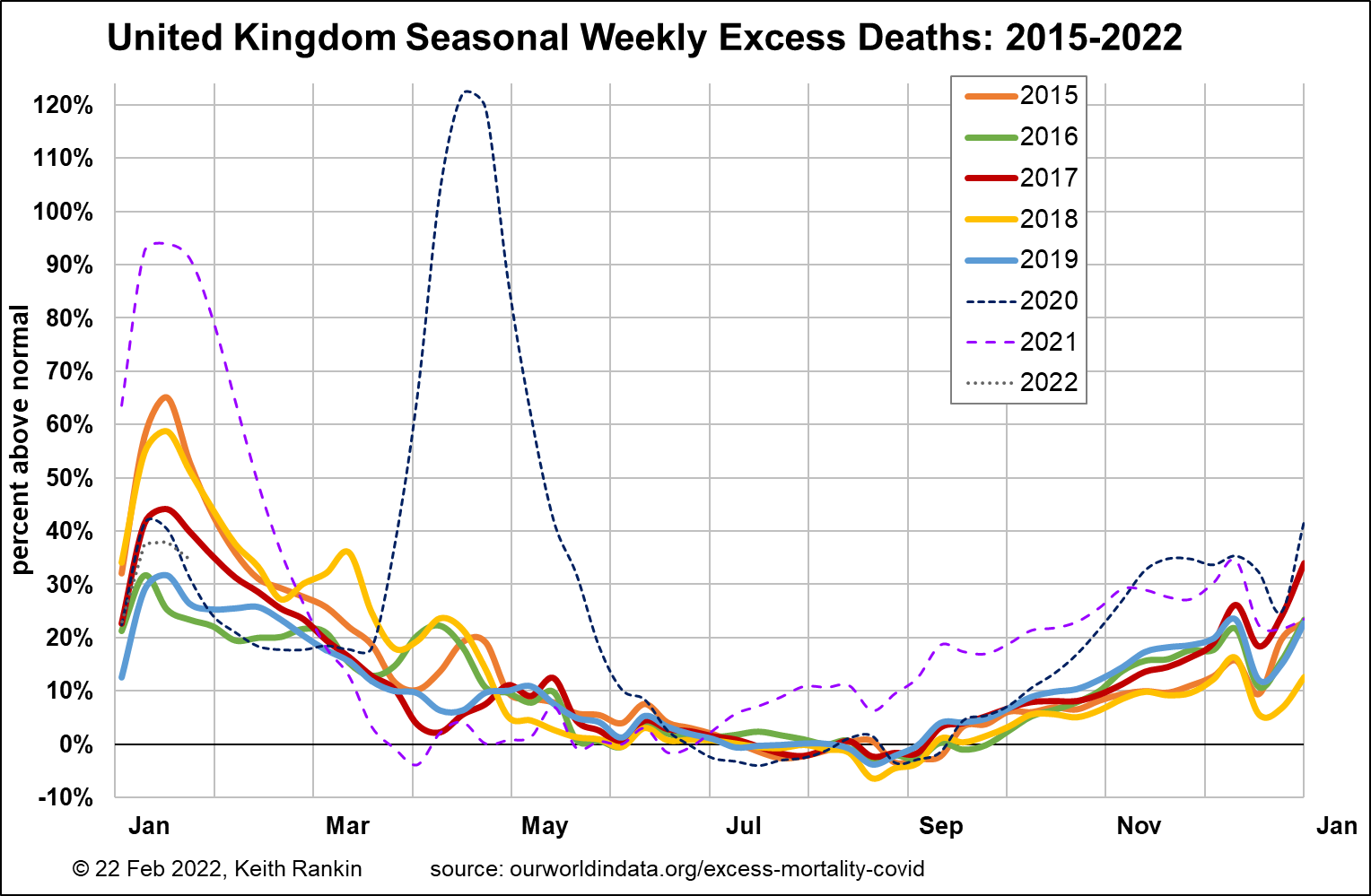
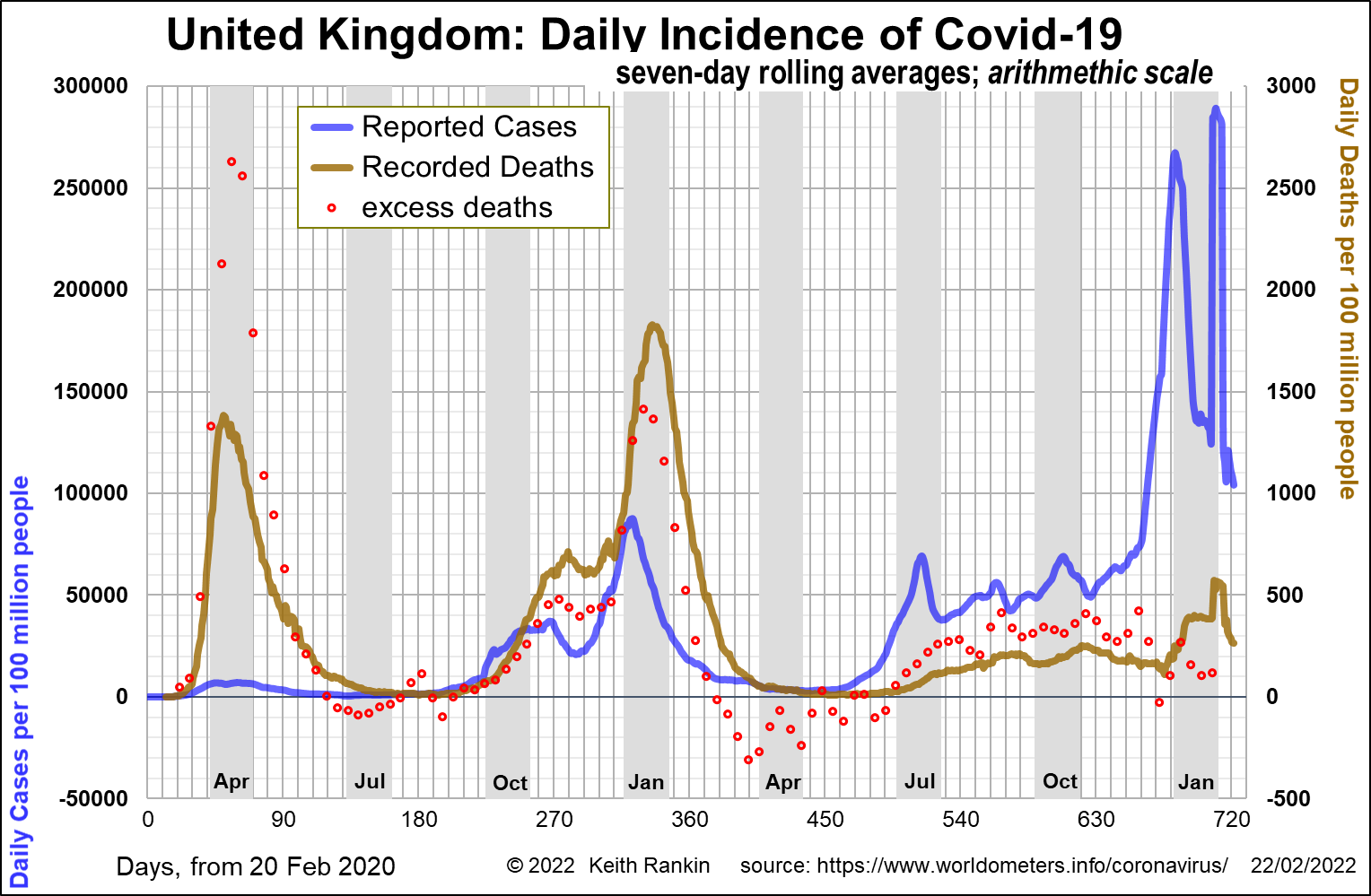
The United Kingdom was among those countries really stung by the first European wave of the novel coronavirus infection that we call Covid19. It then followed the second European wave in the late autumn of 2020, with deaths peaking in January 2021.
In United Kingdom, we see four years where seasonal influenza drove January death rates to in excess of 40 percent above summer mortality norms; 2015, 2017, 2018 and 2020. In January 2016 and January 2019, the seasonal mortality peaks will have been mainly due to endemic ‘colds’. The common cold is a fatal illness, though typically like ‘the straw that broke the camel’s back’.
As noted by Dr Chris Smith on RNZ (Saturday Morning, Covid-19 science news) last Saturday, excess deaths during the Omicron covid wave are similar to those of a comparatively good influenza season.
The United Kingdom had a Delta problem comparable to that of Norway, though the factors causing death were probably more complex, including more ‘younger’ people with comorbidities. Norway generally has a healthier population than does the United Kingdom.
Note that, more than any other country, the United Kingdom has ‘blips’ in its reporting of deaths around the ‘festive season’.
South Africa
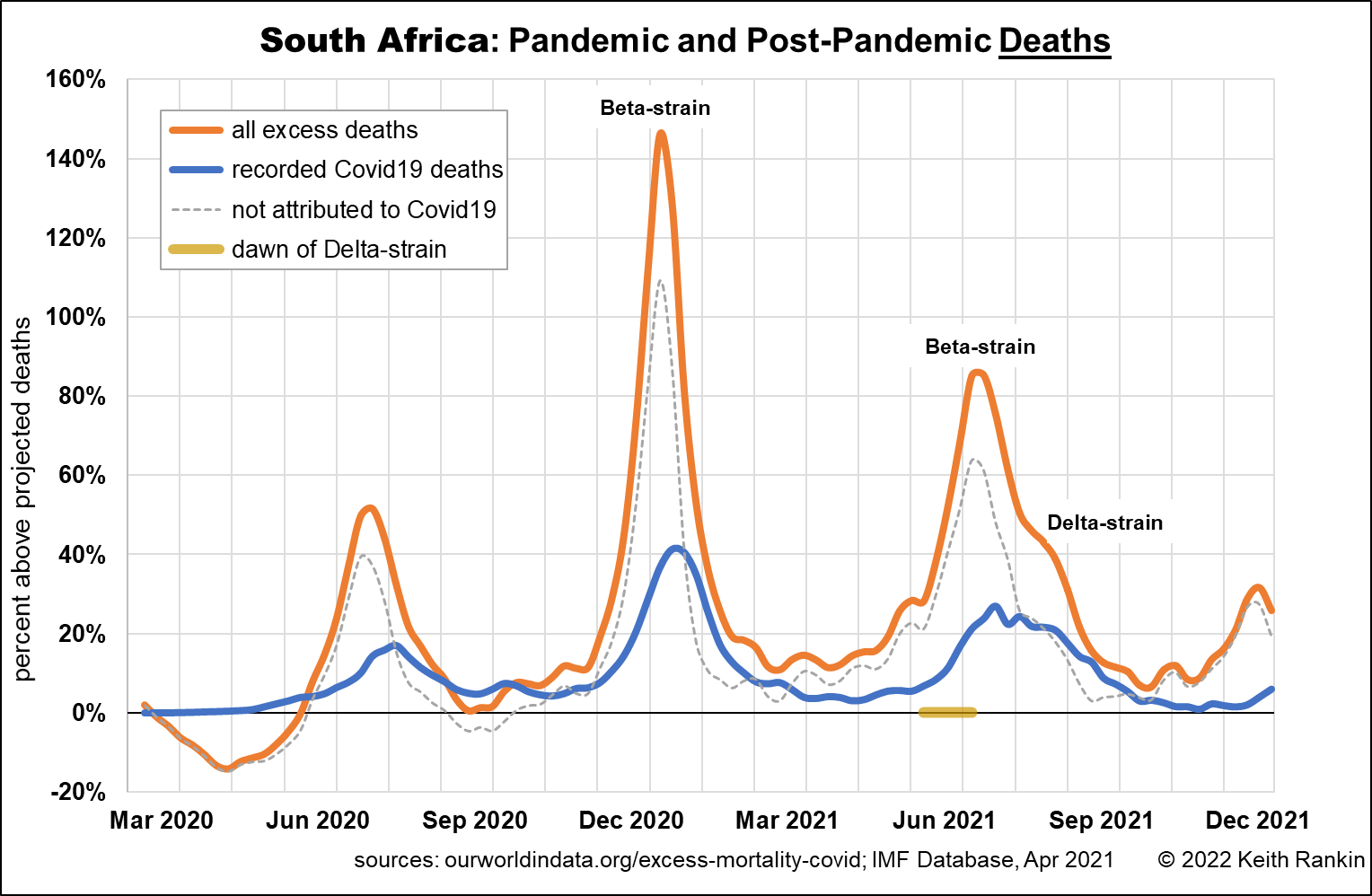
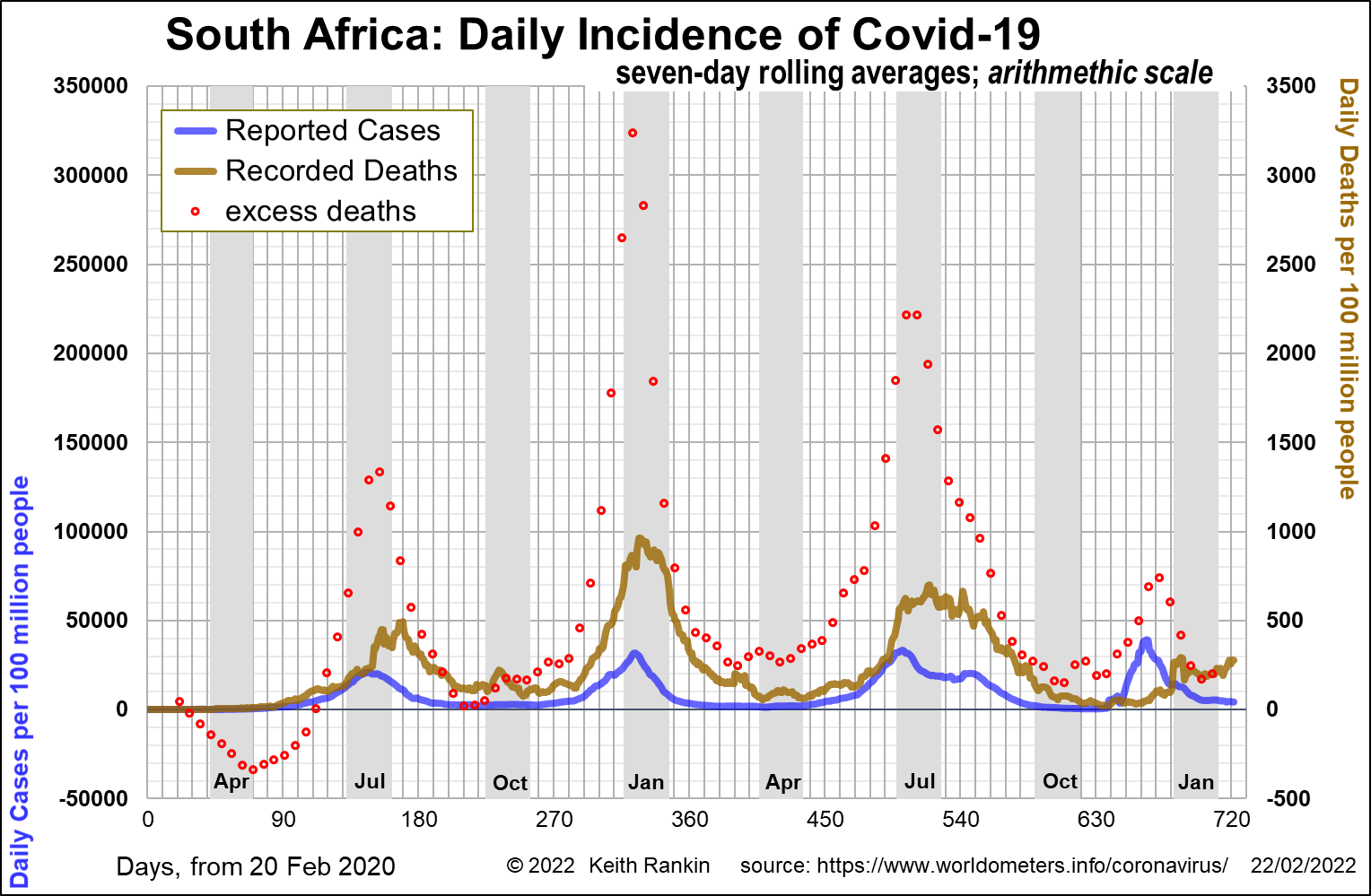
South Africa is more complex, in part because it was home to the dangerous Beta strain of Covid19. Also, South Africa went through an extraordinary set of lockdowns and other measures in early 2020 which left its population highly vulnerable to the next wave of covid, which came in the summer of 2020. Delta hit South Africa during an intense Beta wave. Thus, Delta’s impact was originally muted.
Delta’s main impact in South Africa was in December 2020, the same month that Omicron – probably from Botswana – became a thing. This wave of Delta caught South Africa unawares, with few recorded Covid19 deaths. It was probably most prevalent in some of the poor townships where most covid victims died at home, undiagnosed.
Excess deaths fell rapidly in South Africa, just in the weeks that Omicron rapidly overtook Delta as South Africa’s most prevalent variant.
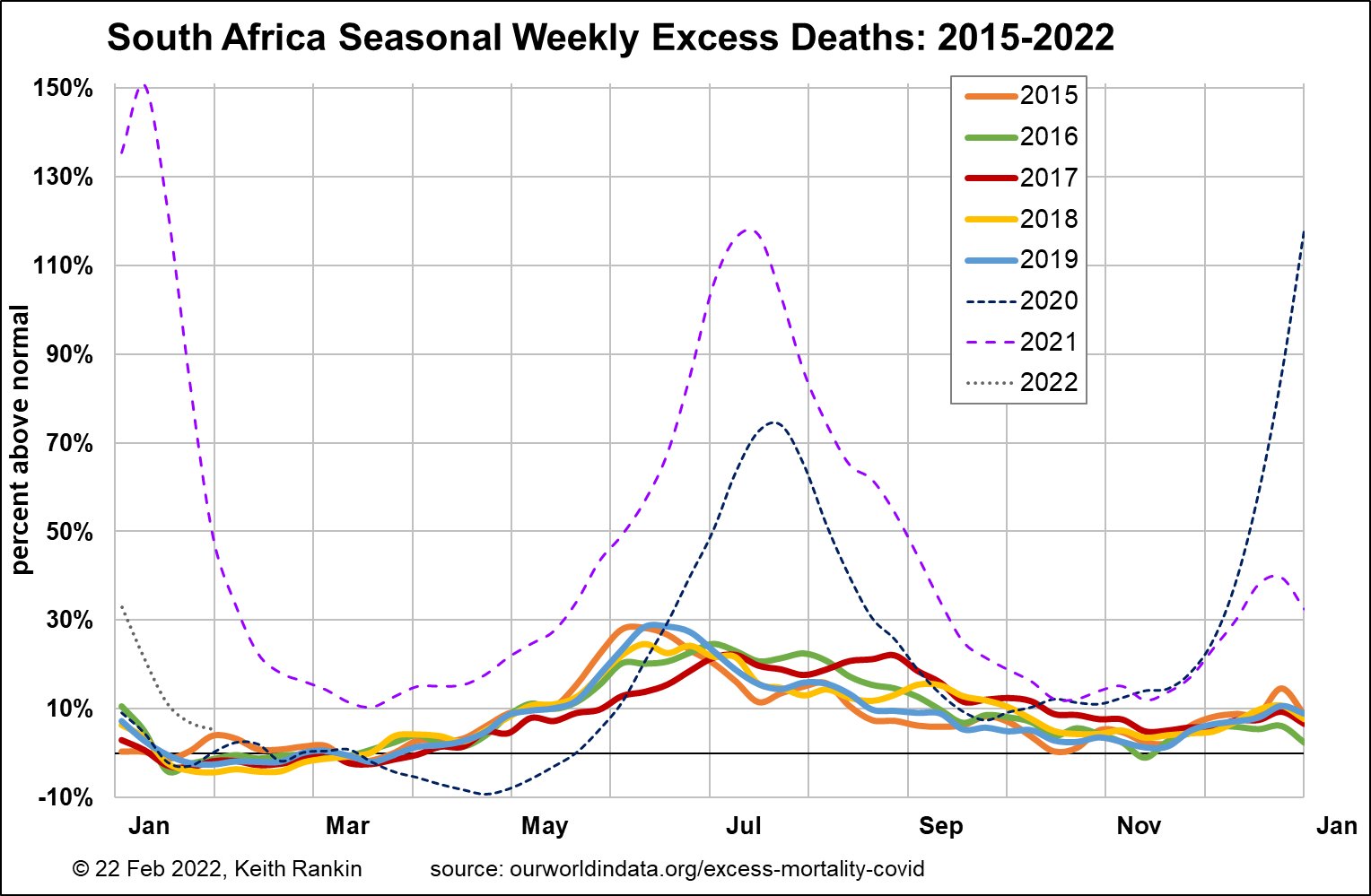
We see that South Africa’s four death waves were basically six months apart, each mid-winter and each mid-summer. The last wave – the Delta death wave – was significantly lower than the previous three wave, no doubt due to raised levels of natural immunity. There was no Omicron death wave.
South Africa is clearly a country that was heavily vulnerable to Covid19; far mor than those countries that encountered Covid19 just after their winter flu and cold seasons. Also, interestingly and unusually, South Africa is most vulnerable to influenzas and colds in June, early in winter.
South Africa’s experience is not unlike that of Colombia, though South Africa has a much lower life expectancy than Colombia. Both countries appear to have had inherent vulnerabilities to a novel coronavirus; vulnerabilities substantially exacerbated by their similar experiences of stringent public health mandates in the early months of the pandemic.
*******
Keith Rankin (keith at rankin dot nz), trained as an economic historian, is a retired lecturer in Economics and Statistics. He lives in Auckland, New Zealand.

