Source: The Conversation (Au and NZ) – By Mark Davies, Laboratory Head, Doherty Institute, The University of Melbourne
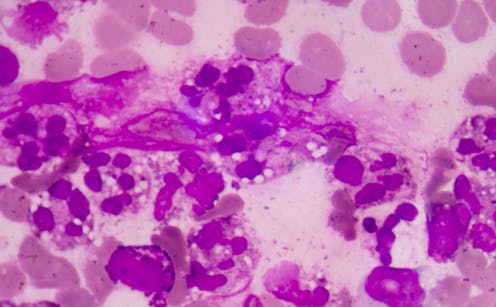
Group A streptococci, also known as “strep A”, has been on the rise around the world with a new strain reported in the United Kingdom and Europe. This variant has been linked with surges of scarlet fever and a marked increase in life-threatening invasive strep A infections.
Now genomic research by our team of scientists has identified this new strain in the Australian community for the first time. In parallel, we have seen an increase in invasive strep A cases across New South Wales, Queensland, Western Australia and Victoria.
Strep A is a common bacteria carried by people primarily in their throat. It can cause mild illness including sore throat, scarlet fever (named for the red rash it causes) and impetigo (“school sores”). But it can also cause “invasive” disease, such as sepsis. Repeated strep A infections can lead to other serious conditions including acute rheumatic fever and rheumatic heart disease.
We investigated the genetic composition of the new strep A strain called “M1UK” and zeroed in on what makes it different to the previous strain.
Read more:
Strep A: three doctors explain what you need to look out for
What we know about strep A
Strep A only infects humans, with around 10% of school-aged children carrying it. It causes more than half a million deaths worldwide per year.
We’ve known about the bacteria for over 100 years and it was a major cause of childhood death in the 19th and early 20th centuries. But it’s been less of a public health threat since antibiotic medications were developed to treat it. In the 1980s, one type of strep A strain called “M1” emerged as the major cause of invasive strep A infections in high-income settings.
Over the last decade, resurgence of scarlet fever strep A infections has been reported in the United Kingdom and China.
Invasive infection is rare. But when it occurs, the death rate can be as high as 20% of those infected.

Shutterstock
What’s different about this strain?
The M1UK variant of strep A was first reported in the UK in 2019 and identified using genomics – the study of the DNA sequence to identify changes in the genetic makeup of an organism.
UK scientists identified that the M1UK variant expressed up to five times more of a specific strep A toxin than the previous M1 strain, but they weren’t sure how. This toxin, originally termed the “scarlet fever toxin”, is associated with the development of invasive strep A by short-circuiting the host’s immune system.
Our laboratory team went about trying to understand which changes in the bacteria led to this increased expression.
We looked at the genetic code of the strep A M1UK variant and compared it to previous ones. We found a number of mutations, one of which was located near the toxin gene.
Then we worked backwards to repair that change and see how it affected the amount of toxin expressed. In this way, we identified the mechanism of how M1UK strep A became toxin supercharged.
Will we see more dangerous strep A strains?
Genomics helps us identify and track bacterial variants. Then scientists need to use that knowledge within a biological context to figure out how a strain is gaining competitive advantage to become dominant over a previous strain – as M1UK has in the UK.
It’s possible this new strain of strep A is better at transmitting from person to person, but we’ll need more research to know if this is the case.
Invasive strep A is now a notifiable disease
Invasive strep A infection was added to Australia’s National Notifiable Diseases List in July 2021, paving the way for it to be formally recorded across states and territories. This means that detected invasive strep A cases get reported to a central registry so authorities can keep track of outbreaks and case numbers.
Our researchers will have access to a repository of national strep A strains. We will be piloting a national strep A genomic surveillance program within the AusPathoGen program, which will speed up our ability to identify and track emerging strep A variants.
We’ve seen how this type of genomic research has helped track COVID changes and guide public health response. By undertaking this pilot program with public health partners, we aim to build a national invasive strep A surveillance framework.
Read more:
Strep A cases are rising. We must remember our earliest hygiene lessons as vaccine trials continue
How can people protect themselves?
Invasive strep A is still extremely rare, so there’s no need to panic – but we shouldn’t be complacent either.
Basic hygiene practices and staying away from other people when sick remain important for preventing spread.
Kids or the elderly are more likely to get invasive disease, so if you note symptoms such as high fever (especially with a skin rash), severe pain from an infected skin sore, and any difficulties with breathing then you should go to your local hospital’s emergency department or consult a GP immediately.
Antibiotics are highly effective at treating infection, provided they are available.
We also need to think about alternative ways of controlling infection. Australian scientists are at the forefront of efforts to develop a global strep A vaccine.
Read more:
Antibiotics shortages: what’s causing them and how countries can minimise the impact
![]()
Mark Davies receives funding from the National Health and Medical Research Council of Australia.
– ref. Genomics has helped identify a new strep A strain in Australia – and what has made it dangerous – https://theconversation.com/genomics-has-helped-identify-a-new-strep-a-strain-in-australia-and-what-has-made-it-dangerous-200815
