Source: The Conversation (Au and NZ) – By Tony Blakely, Professor of Epidemiology, Population Interventions Unit, Centre for Epidemiology and Biostatistics, Melbourne School of Population and Global Health, The University of Melbourne

COVID case numbers are tracking up in Australia, with an average of 57,000 new cases recorded each day.
New South Wales is recording around 21,000 cases a day, the highest number in two months, while Victoria has around 10,000 a day.
Some states may be at or close to the peak of this latest wave, with their growth in cases slowing, while others continue to track upwards.
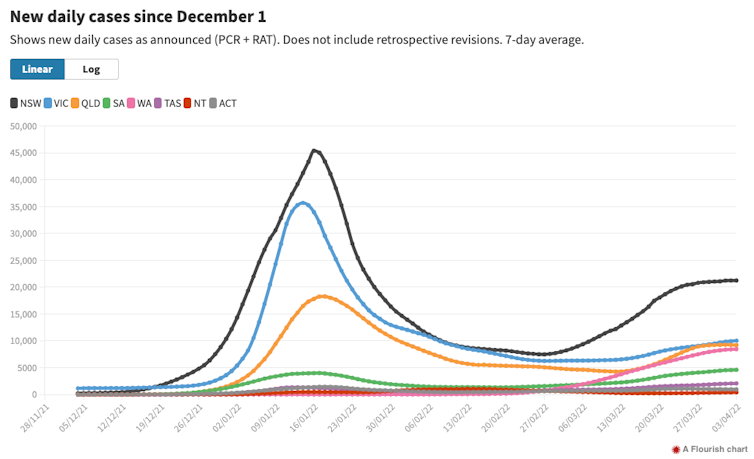
COVID19data.com.au
Rising case numbers are due to three factors:
-
Omicron BA.2 – a sub-variant of the original Omicron – has become the dominant strain. BA.2 is more infectious than old Omicron, including among the vaccinated
-
mask mandates in many settings were dropped in New South Wales, Victoria, the ACT and Queensland in late February and early March
-
we’re out out and about more, with a greater number of social contacts each day.
Omicron BA.2 case numbers are unlikely to reach worrying heights requiring reinstating restrictions.
We do, however, need to be ready to respond to new variants which may be more virulent (think Delta or worse, with high hospitalisation and death rates) and highly infectious (think Omicron or worse).
Read more:
BA.2 is like Omicron’s sister. Here’s what we know about it so far
Does it matter that case numbers are currently rising?
Yes. Older people and those with underlying health conditions are at higher risk of hospitalisation and death, and want to avoid COVID infection. For them, it’s important to:
- keep up-to-date with vaccinations (given they wane in effectiveness)
- wear high-quality masks when around other people indoors
- ask visitors to have a rapid antigen test before visiting.
But for the younger and vaccinated, Omicron infection is likely a mild illness.
We don’t yet know how people with Omicron are affected by long COVID. But given it causes less severe disease than Delta and is more of an upper respiratory illness and less likely to infect the lung tissue, long COVID is likely to be less common and less severe.
Therefore, as long as the rising hospitalisation rates do not get to a level that stretches the health system, we don’t need to reinstate restrictions again. Currently, hospital numbers are well shy of overburdening the health system.
There are advantages to Australia’s high levels of immunity through vaccination and infection with Omicron. An infection adds to your vaccine-induced immunity and makes you less likely to be reinfected.
Could lockdowns come back for BA.2?
Greater restrictions are unlikely to be needed to control Omicron BA.2. But we can never say never with COVID-19. If hospitalisation numbers do increase to a level that stretches health services, we may need to turn back on some public health measures. However lockdowns are still unlikely for BA.2.

Shutterstock
It wouldn’t take many additional public health restrictions to keep case numbers in check, given our increasing population immunity. It could mean, for instance, returning to mask mandates for all indoor environments and encouraging people to work at home.
We do, however, need to be prepared for new variants.
Read more:
COVID mask mandates might be largely gone but here are 5 reasons to keep wearing yours
How easily could a new variant spread?
New variants muscle out existing variants because they are either innately more infectious, or have some immune escape, meaning vaccines or previous infection offer less protection.
But there is no natural selection advantage based on innate virulence (how likely it is to cause severe illness, hospitalisation and death). We just don’t know what the next variant will bring.
We’re lucky the variant that came along just as we were largely vaccinated and ready to open up to the world was Omicron with lower virulence. We may not be so lucky next time.
For arguments sake, let’s imagine a new variant arrives in mid-2022 that is as or more virulent than Delta.
We would expect this new variant to not spread as fast, not infect as many people and not hospitalise and kill as many people as if the variant had arrived in 2020. Our immunity from vaccines and natural infection, while not perfect, should slow its spread and result in less serious illness if infected.

Shutterstock
However, a new variant could still stress our health systems and society again. So if a new variant arrives that is innately more severe (causing more hospitalisations and death despite our high vaccination and Omicron infection rates), we will probably have to turn some restrictions back on, such as wearing masks indoors and working from home if you can.
We don’t want to have lockdowns again. To avoid that, we need to use the other tools in our toolbox.
What do we need to do to prepare?
If we want to keep society open and ticking along in the face of a new, more infectious and more severe variant, we need planning and action in four key areas:
-
ongoing improvement of ventilation of indoor spaces
-
large stockpiles of rapid antigen tests (RATs)
-
a large stockpile of masks. KN95 and N95 masks reduce a person’s risk of COVID infection by 83%, compared to 56-66% or so for cloth and surgical masks
-
early access to next-generation vaccines that will better protect us against new variants. These should arrive later this year or in 2023 and will be a game-changer for protection.
Distributing ten high quality masks to all Australians aged 12 and older would also be a game changer in a serious outbreak. But to enable this, federal and state governments will need to stockpile 200 million or more KN95 or N95 masks.
Let’s not repeat the policy failure of not ordering RATs in 2021, and be better prepared.
![]()
Tony Blakely consults for Moderna. He has received funding for COVID-19 research from the Victorian Government and an anonymous philanthropist.
– ref. COVID cases are rising but we probably won’t need more restrictions unless a worse variant hits – https://theconversation.com/covid-cases-are-rising-but-we-probably-wont-need-more-restrictions-unless-a-worse-variant-hits-179969
