Source: The Conversation (Au and NZ) – By Sophie Hickey, Postdoctoral researcher, Charles Darwin University

Many Australian women rely on and trust maternity services to see them through pregnancy, labour and the early stages of new parenting.
But for First Nations women, these same services can be confronting and can result in poor outcomes. Many women must travel far from family and community to birth. And if they don’t, they often feel misunderstood and judged by mainstream health services.
There is another way. Birthing on Country means First Nations women give birth on their ancestral country. It acknowledges First Nation peoples’ continued ownership of land and unique birthing practices.
What can Birthing on Country services do?
Birthing on Country services centre First Nations values, and are designed to meet First Nations people’s social, emotional, cultural and health needs. The services are embedded within larger health service networks.
Our team works in partnership with First Nations communities to deliver Birthing on Country maternity services that address health inequities.
Our partners in one urban setting saw a profound reduction in preterm birth and increased antenatal attendance and breastfeeding.
Read more:
Birthing on Country could deliver healthier babies and communities
This was achieved through integrating within a wraparound system of care, designed as a one-stop-shop in an Aboriginal community controlled setting.
It also involved redesigning the service using a successful blueprint that prioritises investing in the workforce, strengthening families’ capabilities, and embedding First Nations governance and control in all aspects of maternity service planning and delivery.
However, Birthing on Country services are yet to be trialled in regional and remote Australia. So there is much work to do to ensure all First Nations women can access these services.
Here are five ways to work towards this:
1. Acknowledge safe childbirth is a human right
Australia is a signatory to the United Nations Declaration on the Rights of Indigenous Peoples which states Indigenous people have the right to:
- quality, culturally safe health care
- be self-determining and participate in the design of health services
- include and revitalise cultural practices, languages, and medicines.
Birthing on Country services are one example of how this can be achieved.
Commitment to uphold the UN declaration requires resourcing and monitoring to support and celebrate the world’s oldest midwifery practices and cultures.
2. Acknowledge how health systems fail First Nations people
First Nations people and cultures are wrongly blamed as the cause of health inequities, rather than focusing on how the health system continues to fail First Nations families.
Racial bias has been identified as a contributing factor in First Nations maternal deaths. This includes health services dismissing women’s concerns and turning them away from hospital when seeking care – even when they have life-threatening symptoms.
This can make First Nations families feel unsafe and uncomfortable accessing maternity health services.
Large organisations make Western ways of “knowing and doing” dominant in every work practice. This often results in institutionalised racism and dismisses other forms of knowledge suggesting we should or could be doing things differently.
Read more:
Microaggressions aren’t just innocent blunders – new research links them with racial bias
3. Ensure there is ‘nothing about us without us!’
Australia’s health system was designed to serve those who designed it.
First Nations people have been explicitly excluded from decision-making about the services provided to them.
First Nations people want and need to be at the decision-making table, and ensure “nothing about us” is decided “without us”.
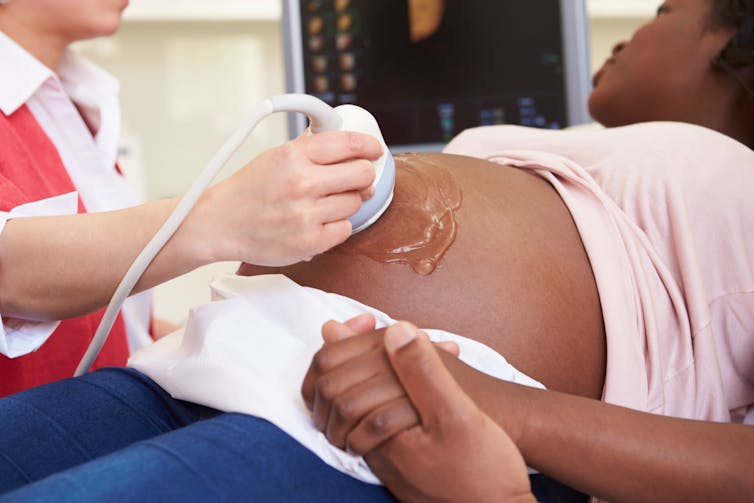
Shutterstock
Participatory action research is one evidence-based way to work collaboratively with stakeholders to respond to needs identified by the community.
First Nations people value the process as it aligns with principles of self-determination and equity. And it privileges the voices of those often marginalised in research.
Engaging community in design, implementation and evaluation of maternity services brings local knowledge, community activation and investment that leads to lasting change.
4. Recognise how First Nations peoples can improve health care for everyone
Our colleagues in Aotearoa (New Zealand) found maternity systems that privilege whiteness cannot provide equitable health care for all.
All people can benefit from ethical knowledge systems that have safely guided childbirth and the flourishing of First Nations people for millennia.
Relationality – being connected with all human and non-human beings – is at the centre of First Nations values, ways of knowing, doing and being. It ensures our responsibility to be in good relations with each other, whether with community, Country or our research partners.
The current system does not embed relationality in its design; rather encourages capitalism and competition for scarce resources over genuine partnership and equitable care.
Read more:
Why we need to support Aboriginal women’s choice to give birth on country
Our task is to re-centre good relations in our everyday work to make health and wellness gains. We do this by:
- ensuring our work is community-driven
- using methodologies that represent First Nations views
- presenting and defending findings at community forums
- ensuring our research leads to action at the local, state and national level.
5. Share findings in accessible ways
The Caring for Mum on Country project is a community-driven action research project piloting doula (birthing companion) training and exploring reproductive health literacy.
It has shown the power of grassroots community activation in finding Yolŋu solutions to local needs.
Charles Darwin University researchers Sarah Ireland (a co-author of this article) and Ḻäwurrpa Maypilama (in partnership with the Australian Doula College and Yalu Aboriginal Corporation) used community action research to pilot First Nations doula training, locally known as djäkamirr–caretakers of pregnancy and birth.
They made a documentary about their project:
Film is an impactful way to discuss research. Finding creative and accessible ways to share research findings is imperative to bringing learnings to people who can benefit from and enact change.
Health inequities in childbirth will persist until health systems relinquish control and acknowledge the value of First Nations knowledge systems centred on relationality and wellness.
We must work in partnership with First Nations communities to redesign health services and work differently with communities in their journeys to implementing Birthing on Country maternity services.
![]()
Sarah Ireland receives funding from NHMRC Partnership Grant 2021: “To Be Born Upon a Pandanus Mat” APP2010289.
Yvette Roe receives funding from NHMRC .
CI A Prof Yvette Roe, NHMRC Centre of Research Excellence: 2020 Redesigning maternal, newborn and child health services for the best start in life for First Nations families. APP1197110
CI A Prof Yvette Roe, NHMRC Partnership Grant 2021: “To Be Born Upon a Pandanus Mat”. APP 2010289
Sophie Hickey does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
– ref. Birthing on Country services centre First Nations cultures and empower women in pregnancy and childbirth – https://theconversation.com/birthing-on-country-services-centre-first-nations-cultures-and-empower-women-in-pregnancy-and-childbirth-170641
