Source: The Conversation (Au and NZ) – By Fiona Russell, Senior Principal Research Fellow; paediatrician; infectious diseases epidemiologist; vaccinologist, The University of Melbourne

Eighteen months into the COVID-19 pandemic, some countries that have achieved high vaccination coverage in adults have started vaccinating adolescents aged 12-15.
Drivers to vaccinate children and adolescents include building confidence to open schools, preventing severe disease, and reducing transmission in all ages to achieve “herd immunity”.
But in most countries, including Australia, vaccination of the highest-risk groups is not nearly complete. So does it make sense to vaccinate children and adolescents at this stage?
COVID-19 in children
COVID-19 is less severe in children and adolescents; most have mild infections or are asymptomatic.
Studies have found multisystem inflammatory syndrome and long COVID to be uncommon after COVID-19 infection, especially in young children.
Newborns and children with other medical conditions are at higher risk of severe disease. But with the level of medical care in Australia, even the more vulnerable children have a very low risk of dying.
Given the increased risk in children with underlying health issues, there may be benefit to vaccinating these children over 12, and a strong case for 16- to 18-year-olds.
But as increasing age is the biggest risk factor for severe disease, vaccinating older people should remain the priority.
Are COVID vaccines safe for kids?
Common side-effects seen in a clinical trial of the Pfizer vaccine in 12- to 15-year-olds included injection site pain (up to 86% of participants), fatigue (up to 66%) and headache (up to 65%). These were mild to moderate in severity and short-lived.
However, two more serious, related conditions — myocarditis (inflammation of the heart muscle) and pericarditis (inflammation of the heart lining) — have been identified in safety surveillance in the United States, Canada and Israel following mRNA vaccines (Pfizer and Moderna).
The highest rates are in men under 25 after the second dose. Based on US data up to June 11, for boys aged 12-17, the rate was 66.7 cases per million second doses.
This is more than double the estimated risk of thrombosis with thrombocytopenia syndrome (TTS) following the AstraZeneca vaccine, although myocarditis and pericarditis are less severe.
Most of the 323 cases recorded in the US data went to hospital; some needed intensive care, but the vast majority fully recovered.
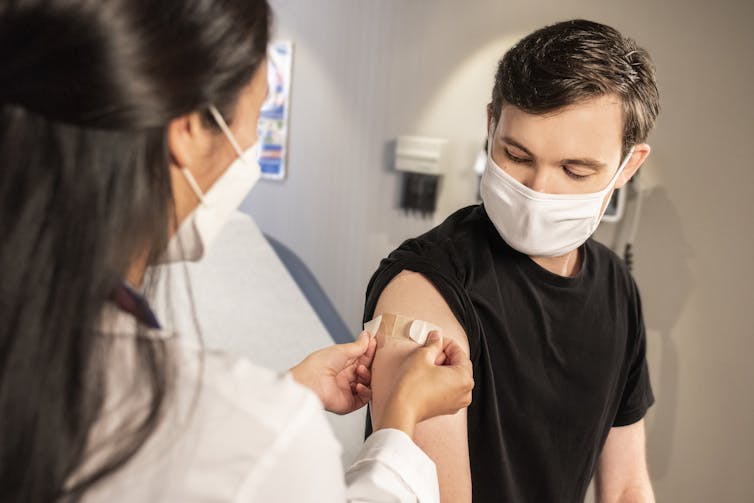
ADC/Unsplash
What are other countries doing?
These heart conditions may be triggered by autoimmune responses following mRNA vaccines in susceptible young people. Given immune responses are higher in adolescents than adults after vaccination, experts are considering altering the vaccine dosage or schedule in this age group.
Israel is now weighing up a single dose for adolescents, as one dose produces a good immune response, and almost all cases of myocarditis or pericarditis believed to be associated with the vaccine occurred after the second dose.
In the US, the risk of COVID-19 was judged to render the benefits of the existing adolescent vaccination program substantially greater than the risks from vaccination.
In the United Kingdom, infections with the Delta variant have increased, particularly in older adolescents in hotspots. However, the UK has decided not to vaccinate children under 18 just yet, as there would be little direct benefit in this age group.
Vaccine safety must be paramount, especially where the risk of COVID-19 is low, such as in Australia. Although Australia hasn’t yet approved a COVID-19 vaccine for this younger age group, any risk/benefit calculation would be based on our local context, as we’ve seen with the AstraZeneca vaccine.
What about outbreaks in schools?
The most profound effect on children and adolescents during the pandemic has been the impact of school closures on learning, socialisation and emotional development, especially in children with special needs or mental health issues.
The US and Canada are vaccinating adolescents partly to build confidence for returning to school.
School outbreaks do occur and are proportionate to the degree of community transmission. In Australia’s current Delta outbreak, we’ve seen very few school-related infections.
But it’s important to understand adult staff are responsible for most transmission in schools. And most transmission — linked to schools or generally — occurs in households. We’ve seen this even in the UK with the Delta variant.
A Scottish study with data up to February found the highest risk factor of infection in people at risk of severe COVID-19 was the number of adults in their household. Living with children was not a risk factor.
Vaccinating adults, parents and school staff will be key to preventing infections in children and schools.
Do we need to vaccinate children and teens to control COVID-19?
Vaccinating large numbers of adults will allow us to prevent deaths and serious illness, and therefore reduce the burden on health systems. That’s the primary goal.
But many countries are also aiming to achieve “herd immunity” through vaccination. High coverage in adults will go a long way to achieving this, but the incremental benefit from vaccinating children 15 and under is still unclear.
In Serrana, a small town in Brazil, where 95% of the adult population (about 75% of the total population) were given two doses of Sinovac vaccine, deaths were reduced by 95%, hospitalisations by 86% and symptomatic infections by 80%. Infections in unvaccinated children and adolescents also went down.
In some countries with adult vaccination rates above 50%, such as Israel, infections have declined overall, suggesting adults play a key role in transmission and preventing infections in children.
In fact, one study in Israel found vaccinating adults did prevent infections in unvaccinated children.
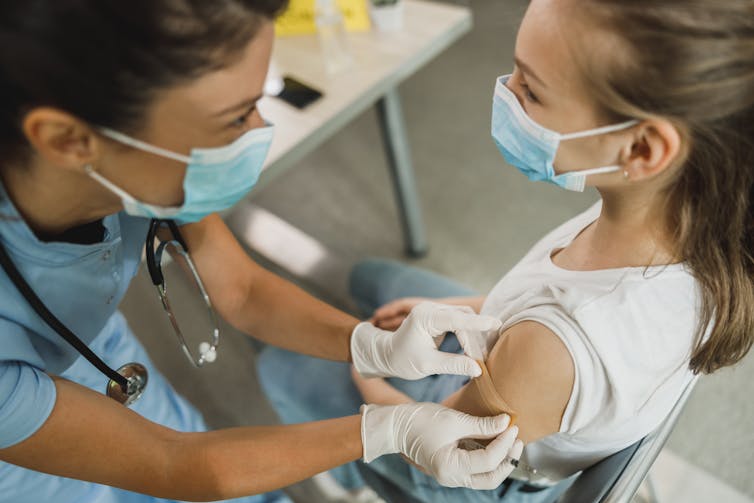
Shutterstock
Let’s keep the focus on adults for now
At this stage, the focus of a vaccination program should remain on attaining high coverage in adults, especially the elderly and those with other medical conditions. We should aim for above 90% coverage in these groups to maximise individual protection and prevent transmission to younger age groups.
Another reason to hold off with adolescents is the fact the global COVID-19 vaccine rollout has been slow and highly inequitable.
The World Health Organization has expressed major concern over higher-income countries beginning to vaccinate children while many lower- and middle-income countries have insufficient supply to vaccinate high-priority groups.
Recommendations for vaccination will evolve. But the top priority right now must be maximising vaccination in adults — both in countries that may have the capacity to vaccinate children, and around the world.
![]()
Fiona Russell receives funding from the NHMRC, the Wellcome Trust, WHO, Bill & Melinda Gates Foundation and DFAT. She advises DFAT and WHO on COVID-19 vaccines in the Asia-Pacific region.
Peter McIntyre receives funding from Novovax Limited for participation in their scientific monitoring committee, and from the Otago Medical Research Foundation and the Health Research Council, New Zealand for research projects – these funds are held by the University of Otago where he is a Professor. He is a member of the World Health Organisation’s Strategic Advisory Group of Experts (SAGE) on immunisation and a Professorial Fellow at Australia’s National Centre for Immunisation Research and Surveillance,
Shidan Tosif does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
– ref. Let’s hold off vaccinating children and teens against COVID-19. Prioritising adults is our best shot for now – https://theconversation.com/lets-hold-off-vaccinating-children-and-teens-against-covid-19-prioritising-adults-is-our-best-shot-for-now-162765





