Source: The Conversation (Au and NZ) – By Holly Seale, Associate professor, UNSW
Health workers are at higher risk of COVID infection and illness. They can also act as extremely efficient transmitters of viruses to others in medical and aged care facilities.
That’s why health workers have been prioritised to get a COVID vaccine when it becomes available in Australia.
But just because health workers are among those first in line to receive a COVID vaccine, it doesn’t necessarily mean they all will.
Read more: Australia’s vaccine rollout will now start next month. Here’s what we’ll need
Our health systems represent a microcosm of the community. Just like in the broader community, there will be health workers highly motivated to get the COVID-19 vaccine, driven by concern about risk to themselves, their family, and their patients. There will also be those who have medical conditions, those that may not be able to get vaccinated, and staff who are hesitant.
There will also be health workers with questions about the vaccine, who perhaps need further support to help them decide.
Reports from the US track vaccine hesitancy among health workers at around 29%. However, it’s important to note different groups have different reasons for COVID-19 vaccine hesitancy; rates and reasons can vary across and within countries.
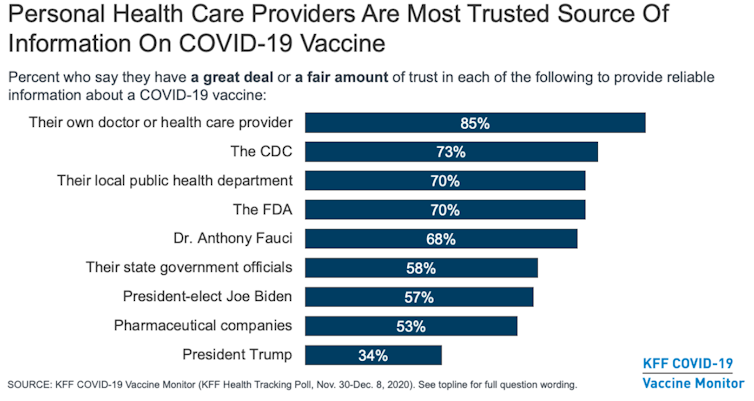
Protecting health workers is critical. Achieving high COVID-19 vaccine uptake among health workers will not only protect these critical staff members, it will also support high levels of uptake among the general public.
Personal health workers are the most trusted source of information on the COVID-19 vaccine.
Health workers can also be complacent and uncertain about vaccination
Decision-making around vaccination can be a complex mix of psychosocial, cultural, political and other factors.
Health workers, just like the broader public, may perceive they are at low risk of acquiring a vaccine-preventable disease. They may have concerns about the safety and effectiveness of a vaccine and/or may find it challenging to get vaccinated.
All these factors may make a health worker reluctant to get the vaccine and communication strategies should be tailored to take these factors into account.
Read more: The Oxford vaccine has unique advantages, as does Pfizer’s. Using both is Australia’s best strategy
How to achieve high and equitable vaccination coverage among health workers
While most health workers understand how vaccines work generally, they may not necessarily be experts across all vaccine types. If we want to ensure they feel comfortable to receive it and advocate for it, then we must address any misunderstanding and concerns health workers may have. This may be focused on the vaccine itself (how it was developed, effectiveness and so on), or the necessity of vaccination.

One strategy that may assist will be to work with middle managers, as they are influential, trusted and can act as vaccine advocates and agents of change. They may also play a role addressing questions or concerns where they arise. If a COVID vaccine becomes an occupational requirement for health workers, hospitals and other organisations need to include middle managers in the development and roll-out of programs. They can then help ensure staff members understand the rationale for the mandate, which staff members are targeted and why.
Investing in the staff responsible for delivering vaccines in the workplace, as well as other potential vaccine allies such as managers, can help reduce COVID vaccine hesitancy among health workers. That will benefit all of us.
– ref. It’s crucial we address COVID vaccine hesitancy among health workers. Here’s where to start – https://theconversation.com/its-crucial-we-address-covid-vaccine-hesitancy-among-health-workers-heres-where-to-start-152977




